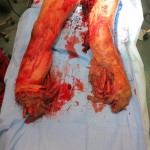
Ara K., a 14-year-old girl, along with her sister and cousin, were riding in a civilian bus when it ran over an improvised explosive device (IED). Although the site had recently been discovered and cleared, a new IED had already been replaced in the same location.
All passengers on Ara K.’s side of the bus were injured or killed. Doctors attempted to revive her cousin at the forward operating base, but both he and Ara K.’s sister died.
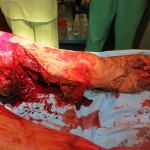
Ara K. suffered massive damage to both legs. Surgeons performed a below-knee amputation on her right leg, but her left leg was more severely damaged. With skin and soft tissue loss, a below-knee amputation was not feasible for her left leg. Posteriorly, large areas would have had near-exposed bone because there was not enough tissue for coverage.
During hurried discussion, one of her surgeons stated, “If we shunted the left leg, it would have been to a high below-knee amputation [due to the soft tissue damage around the knee] and I don’t know how helpful that would be.”
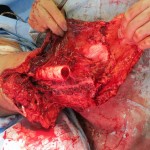
Surgeons ultimately decided to perform an above-knee amputation. Ara K.’s injuries were so proximal, surgeons obtained control of her femoral artery just proximal to the bifurcation and passed vessels loops around it in case she started to hemorrhage massively from her wounds. Care was taken to keep the tourniquet in place and prep it into the surgical field so that controlled release during surgery could be performed.
Ara K. had damaged and thrombosed vasculature just distal to the level where surgeons made the bony amputation cut. The surgeons had to take more muscle medially in order to debride her injury appropriately. They decided to retain as much viable muscle as possible together with her flap, but in the end had to shorten the femoral cut even more because of concerns that the flap was too thin over the end of the femur. They felt that leaving only viable skin over the distal stump would lead to more complications with eventual prosthesis fitting.
In the operating room, Ara K. was given 1:1 transfusions of fresh frozen plasma and packed red blood cells, and surgeons did not have to use proximal control to stop the bleeding.
Ara K. was maintained for a week at the forward base hospital for stabilization of both her lower extremity injuries and other issues related to the blast. She was ultimately transferred in stable condition to the local hospital for completion of care.
In above knee amputations, what is the utility of myodesis with consideration of future mechanical function and prosthesis fitting?
In rural Afghanistan, like most austere environments, prosthesis fitting is quite difficult. There is a national program that is provided, but the waiting list can be quite long. If NO prosthesis services are available, would that change surgeons’ preferences for amputation level decision making? In this case would you have given the “high below-knee amputation” a chance before converting to an above-knee amputation?